- Home
- Types & Treatments
- Ovarian Cancer
- Treatments
Ovarian Cancer
Ovarian Cancer Treatment
Treating ovarian cancer includes both surgery and chemotherapy. Your doctor may recommend molecular and genomic testing to help identify the best ovarian cancer treatments for you.
When you receive ovarian cancer care from us, we tailor an aggressive and precise ovarian cancer treatment program to your particular situation. Your treatment plan is based on your individual needs and the type of ovarian cancer you have. Our multidisciplinary team of gynecologic cancer specialists – gynecologic oncologists, radiation oncologists, pathologists, radiologists – collaborates to customize a treatment plan specifically suited to your needs.
Our gynecologic cancer specialists meet regularly at a tumor conference, where they discuss your ovarian cancer treatment and compare it to nationally established guidelines. This multidisciplinary team of specialists creates and coordinates treatment strategies, as well as ovarian cancer diagnosis for the most advanced ovarian cancer care.
During your monthly visits, your team will test you for the tumor marker CA-125, a protein in your blood that is associated with ovarian cancer. Tumor markers help your doctor evaluate the effectiveness of your treatment for ovarian cancer.
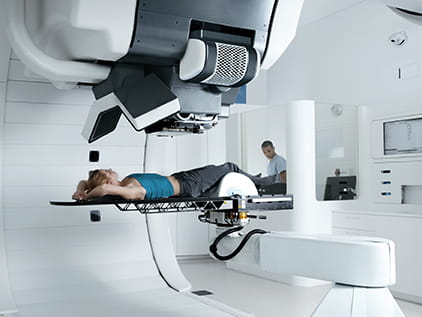
Proton therapy in Kansas City
Receive lifesaving proton therapy treatment from the region's most experienced team of proton experts.
Ovarian cancer treatment options
Surgery is the primary treatment for ovarian cancer. During surgery, your doctor will remove both ovaries, the uterus, fallopian tubes and any other tissue affected by cancer. If it is apparent the cancer has spread, other organs may be partially or completely removed as well.
The gynecologic oncology surgeons at The University of Kansas Cancer Center are highly skilled and nationally recognized. As an academic medical center, we treat a high volume of women with ovarian cancer and have extensive experience treating the disease. Our gynecologic oncologists use the most advanced and minimally invasive surgical techniques available.
Following surgery, you may require chemotherapy to kill any remaining cancer cells. Chemotherapy can be administered in different ways:
- Intravenous delivery of chemotherapy is the most common, and involves inserting a needle into a vein or through an implanted plastic port under the skin.
- Intraperitoneal chemotherapy is another form of chemotherapy delivery. IP delivers concentrated chemotherapy into the abdominal cavity through a catheter or implanted port. The medication circulates inside the abdomen, which allows it to reach more of the internal surface area where cancer is likely to spread. The drugs also get into the blood and travel through the body.

Your best option for beating cancer
The Women’s Cancer Center at The University of Kansas Cancer Center focuses on breast and gynecologic cancers, providing specialized care to women.
Ovarian cancer clinical trials
We encourage you to take part in clinical research trials for ovarian cancer. Many of these studies are initiated by our own gynecologic cancer investigators, who design and implement the research as we work to provide the most advanced ovarian cancer care. Through these trials, we evaluate potential new ways of preventing, diagnosing and treating ovarian cancer.
Woman to Woman mentor program
Woman to Woman at The University of Kansas Health System, a program of the Ovarian Cancer Research Alliance, pairs gynecologic cancer patients with trained volunteer mentors who provide 1-on-1 emotional support and mentoring. From the moment of diagnosis through the end of treatment, mentors help women and their families cope with their diagnosis. They listen, discuss concerns, share experiences, offer support and sometimes just hold a hand.
The program also promotes education and self-advocacy for women in treatment, as well as for their partners, families and other caregivers. Find a mentor and discover tools and resources.
Life After Ovarian Cancer Treatment
Surviving ovarian cancer is a lifelong process. You will need regular checkups. You also may need help with the side effects of treatment. You may want to learn about lifestyle changes that can speed recovery and improve your quality of life.
Our experienced team of doctors, nurses, counselors, dietitians and research coordinators can help you:
- Assess and manage side effects
- Deal with complications
- Give you access to clinical studies
- Make diet and exercise recommendations
- Monitor for cancer recurrence
- Monitor your overall health
- Understand your treatment
You also may wish to visit the Brandmeyer Patient Resource Center for more information.
Women who have survived certain cancers, as well as women who are aging, frequently experience declining estrogen levels that dramatically change their gynecologic health. Our gynecologic specialists now offer a simple, convenient and drug-free solution – MonaLisa Touch® laser therapy. The gentle, safe laser therapy takes only 3 treatments of 5 minutes each, producing rapid and lasting results. The MonaLisa procedure is clinically shown to improve ovarian cancer symptoms, often after just one treatment.
Helpful websites
- American Cancer Society
- Foundation for Women’s Cancer
- National Cancer Institute (part of the U.S. National Institutes of Health)
- National Ovarian Cancer Coalition

We are here for you, woman to woman.
The Woman to Woman program provides 1-on-1 emotional support and mentoring for women who are newly diagnosed with gynecologic cancer.
About the program
Start your path today.
Your journey to health starts here. Call 913-588-1227 or request an appointment at The University of Kansas Cancer Center.