- Home
- News Room
- Patient Stories Search Page
- 100th Proton Therapy Patient Extols Her Positive Treatment Experience
August 17, 2023
Posterior fossa ependymoma. Most people have never heard these words because they describe a rare type of brain tumor, affecting only about 13,000 people in America, most of them children.
Stylee Gray certainly never expected to hear them. Yet in January 2021, at age 19, she was diagnosed with stage ll PFE. “It was just crazy,” she says, recalling her diagnosis. “I thought I was indestructible,” she continues. “I just didn’t want to believe that it was real. You know, you always think, ‘This couldn’t happen to me’ – until it does.”
Since her diagnosis, Stylee has been on a treatment path that eventually led her to the Proton Therapy Center at The University of Kansas Cancer Center, a National Cancer Institute-designated comprehensive cancer center. There, she was the 100th patient treated with this leading-edge form of radiation therapy since the center opened in 2022.
From shocking diagnosis to clear treatment choice
Stylee began experiencing troubling visual changes months before her diagnosis. She first visited an ophthalmologist when she experienced double vision and deteriorating visual acuity. The eye exam detected swollen optic nerves, and she was referred to her primary care physician for a more complete exam. Her doctor quickly ordered an MRI of Stylee’s brain, and within days she received the devastating news that her symptoms were caused by a brain tumor.
After the initial diagnosis, things happened fast. The neurosurgery team at The University of Kansas Health System removed as much of Stylee’s tumor as possible on January 21, 2021.
The excised tumor was examined by a neuropathologist to precisely identify the tumor type, which would determine next steps. Together, specialists in neuroradiology, neuropathology, neurosurgery and radiation oncology met in a tumor board to discuss details of Stylee’s case and treatment planning. By March 2021, Stylee’s doctors knew she had a posterior fossa ependymoma and recommended proton treatment to ensure the tumor was fully eradicated.
Proton therapy is more precisely targeted than traditional X-ray or photon radiation, sparing healthy tissue near the tumor site while helping to ensure that any remaining malignancy is destroyed. Stylee’s tumor was located between her brainstem and cerebellum, crucial brain structures at the back of the head (the “posterior” of the brain) that govern basic functions including respiration, heart rate, balance and movement. By using proton therapy, physicians could deliver radiation with extraordinary precision, avoiding these critical nearby brain regions and reducing any chance of damage that would result in permanent cognitive or functional changes.
“The way they explained it to me is that traditional radiation is like a flashlight, but proton therapy is like a laser,” Stylee says. Since her type of tumor is rare, little data exist about it, but early evidence showed that patients receiving proton therapy had better long-term outcomes with less incidence of the tumor recurring than those who had traditional radiation.
In addition to head and neck cancers, proton therapy can also be used to treat esophageal, liver, lung, pancreas, prostate, bone and other types of cancer. It is especially beneficial for many pediatric cancers.
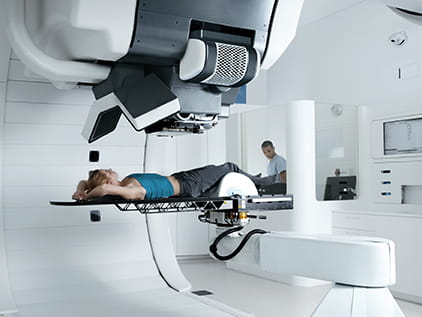
Proton therapy in Kansas City
Receive lifesaving proton therapy treatment from the region's most experienced team of proton experts.
Treatment close to home
When Stylee was diagnosed, the closest proton therapy centers were hundreds of miles away from her Shawnee Mission, Kansas, home. Stylee traveled to Oklahoma City to begin a proton therapy regimen, but after 4 treatments she felt she couldn’t continue. “I did it for 4 days, and then I decided that I didn’t want to do it anymore because I just wanted to be done,” she recalls. “I wanted to pretend that nothing was wrong with me. It was just easier to pretend everything was fine.”
Still in the midst of pandemic protocols, Stylee had little support during her short stay in Oklahoma. She was on her own in an unfamiliar city, healing from brain surgery, and feeling scared. Her doctors reiterated the importance of treatment for long-term survival, but Stylee simply couldn’t cope.
“It was just out of my comfort zone,” she says. “I was really sore from surgery, and I still had a surgical drain, and it was uncomfortable to be strapped to the table for the treatment. My 19-year-old self just wasn’t having it, and I decided that I didn’t want to do it.”
Stylee’s attitude changed when the Proton Therapy Center opened adjacent to The University of Kansas Health System in Kansas City, Kansas. It is the only proton therapy center in the state and in the greater Kansas City region. For Stylee, being close to home with her friends and family nearby improved her outlook and confidence, and as weeks passed, she thought more about the benefits of proton therapy.
“Being closer to where I live was convenient, and I have my support system here. Being close to my friends and fiancé made it so much easier,” Stylee says. In January 2023, Stylee resumed her proton therapy and completed her 25 outpatient treatments on March 10.
Paying it forward
Stylee’s experience completing her proton treatment was so positive she’s now seeking a career as a radiology technologist so she can “give back” to others going through similar experiences. She notes that having reassurance from someone who had been through a similar experience would have helped her feel more comfortable, and that’s what she hopes to do for others.
“The team at the Proton Therapy Center is incredible and made the process so much easier. They began every treatment with a smile, which made it easy to feel encouraged,” she says. “And now I can’t wait to help people the way I’ve been helped. I just want everyone to know how important mindset is. The University of Kansas Cancer Center is full of super-helpful and amazing people that will be there every step of the way.”
Stylee’s physicians will continue to monitor her to ensure any recurrence is quickly found and treated, but Stylee and her medical team are optimistic that her cancer journey is over. Stylee was the 100th patient treated at the Proton Therapy Center, and someday she may be greeting one of the thousands of others who also will find the best possible treatment close to home in Kansas City.
Proton Therapy Center Virtual Tour
Ronny Rotondo: Welcome to the Proton Therapy Center, Kansas City's first proton center and the 39th proton center in the country. I'm Dr. Ronny Rotondo, medical director of the Proton Therapy Center at The University of Kansas Cancer Center.
Ronald Chen: And I'm Dr. Ronald Chen, chair of radiation oncology. Patients of our Proton Therapy Center receive top of the line care from a team of proton experts unparalleled in their region. This includes nationally and internationally renowned radiation oncologists, medical physicists and dosimetrist.
Ronny Rotondo: These specialists, whom we've recruited from across the country will create a customized treatment plan for each patient. Now, we want to take you inside our NCI comprehensive cancer center's proton therapy center. Here is Jessica Lovell to give you a tour.
Jessica Lovell: Hard at work inside the Proton Therapy Center is a pencil thin beam of light giving new hope to cancer patients across the region and beyond.
Jessica Lovell: Hello, I'm Jessica Lovell and welcome to The University of Kansas Cancer Center. I'm standing in what I like to call, the healing hallway that leads back to the proton treatment room. This is where you'll come after you check in at the front desk.
Jessica Lovell: The dogwoods symbolize rebirth but this wood frame is also symbolic. This curve right here, it's intentional. It represents the Bragg-Peak of the proton beam. The precise point where protons stop on a dime to deliver a prescribed dose of radiation to the tumor but not beyond.
Jessica Lovell: So come along, there's must more to show you.
Jessica Lovell: These are the changing areas where you will wait for treatment. There's an area for men and women. Children wait in here too but don't worry, they have plenty of ways to entertain themselves prior, in a family waiting area with TV, animated games, floor art and interactive programming they can take with them, even into treatment.
Jessica Lovell: Now before I show you the treatment room, I want you to understand the prep work that happens first. All proton therapy patients go through a process called CT simulation and treatment planning in the radiation pavilion just down the hall. The CT scan provides imaging to precisely localize the tumor that will require proton therapy. Here, some patients may have a couple of tattoo dots placed on their body to indicate where the radiation beam will be directed.
Jessica Lovell: No worries about any other medical devices you might have, your medical team knows what to consider and that's all part of your personalized plan.
Jessica Lovell: Are you ready to see the vault? That's what we call the treatment room. Come with me.
Jessica Lovell: One of the first things you'll see is this video projection wall. Patients can select from 14 different scenic lighting and surround themes. There are calming scenes as well as jungles, oceans and even outer space. It's all customizable for children and adults. The room temperature is kept at 70 degrees. That's because the proton equipment produces a lot of heat.
Jessica Lovell: Notice the subdued lighting. There's wifi for music. You may bring your own playlist or podcast too. The cyclotron that delivers the proton therapy is behind that locked door. The nozzle delivers the pencil thin beam of protons to the patient. The patient lays on the table, this is when the mask is positioned, if you have one. Images are taken, rotating 220 degrees as the treatment can be delivered from multiple angles and then the nozzle is set. The therapists then exit the treatment room and go to the console area to deliver the treatment.
Jessica Lovell: No worries, cameras and microphones mean the therapists can still see and hear you. Your tumor type determines the number of beams and the length of treatment.
Jessica Lovell: There is absolutely no pain from proton therapy. In fact, you can't even feel the proton beam at all.
Jessica Lovell: While treatment deliver takes just a few minutes, on average it takes 30 minutes to position patients perfectly. There is anesthesia for children and adults who may need it.
Jessica Lovell: Once your treatment is done, you may leave unless it's an exam day. Exams with your doctor happen every five treatments or more often as needed.
Jessica Lovell: Okay, there's just one more thing I wanna show you and that's the proton therapy bell that sits across from the nursing station. When your treatments are done, you'll get to ring it and we'll be right there celebrating with you.
Jessica Lovell: Remember, our medical team is a combination of highly skilled and nationally renowned proton therapy experts available in the region only at The University of Kansas Cancer Center and we thank you for trusting us with your cancer care.
As with all treatments, individual patient results vary. It is important to discuss your treatment options with your healthcare provider.
