- Home
- Outreach & Prevention
- Community Outreach and Engagement
- Masonic Cancer Alliance
Community Outreach and Engagement
Masonic Cancer Alliance
Masonic Cancer Alliance, the outreach network of The University of Kansas Cancer Center, is a membership-based organization that partners with cancer research, care and support professionals to advance the quality and accessibility of cancer prevention, detection, treatment and survivorship in the Heartland.
As the only National Cancer Institute-designated comprehensive cancer center in the region, with a catchment area encompassing the entire state of Kansas and western Missouri, The University of Kansas Cancer Center’s goal is to build a deep understanding of the cancer issues faced by those we serve and respond with tailored solutions. Masonic Cancer Alliance (MCA) is a key partner in this mission to address these specific population-based needs.
One unique characteristic of The University of Kansas Cancer Center’s catchment area is its size of rural inhabitants. About 26% of Kansans live in rural areas, compared to the U.S. average of 19%. People in rural areas are diagnosed with cancer less often but die from it at higher rates. This is in part due to distance to care and lack of access to screenings and other prevention methods.
We created the Masonic Cancer Alliance so members can connect with and learn from each other and work together to improve the health of our state. –Hope Krebill
Executive Director, Masonic Cancer Alliance
Welcome to Bench to Bedside, a weekly series of live conversations about recent advances in cancer, from the research bench to treatment at the patient's bedside. And now your host and the Director of the University of Kansas Cancer Center, Dr. Roy Jensen.
Dr. Roy Jensen: Hi, I'm Dr. Roy Jensen. Thanks for joining us for today's episode of Bench to Bedside. With me today is Dr. Gary Doolittle, Medical Oncologist with the University of Kansas Cancer Center and Medical Director of the Midwest Cancer Alliance, and Hope Krebill, Executive Director of the Midwest Cancer Alliance. Today we're going to discuss the Midwest Cancer Alliance, also known as the MCA, which is the outreach network of the KU Cancer Center. We're also going to be talking about the impact the MCA partnerships have had on rural health in Kansas, so Dr. Doolittle, I'll start with you. Tell us a little bit about the Midwest Cancer Alliance.
Dr. Doolittle: Okay. It's a membership-based organization. It includes physicians, nurses, hospitals that are sprinkled throughout the state. We have some urban partners as well, and basically it's set up to be, as you just said, the outreach arm of the KU Cancer Center. Started over 10 years ago, actually kind of came along at the same time we were working towards NCI designation, and the director of the cancer program at that time had a vision for outreach. You may remember that was you.
Dr. Roy Jensen: That was me. Yes.
Dr. Doolittle: Had a vision for outreach, and this is part of the service we have to our region as an NCI designated center.
Dr. Roy Jensen: So why the focus on rural health?
Dr. Krebill: I'll take that. Kansas is a widely rural community. We have 105 counties across the state. Most of them, smaller populations, and what we know about cancer in rural communities are that cancer is diagnosed less often, and yet people die of it more often. And Kansas is a perfect example with colorectal cancer. We're less likely to get screened in rural communities for colorectal cancer. We are more likely to be diagnosed at a later stage, and more likely to die. And so for us it just makes sense, if that's where we're seeing some of the cancer disparities, we should go out and and try to make a difference. Now, it doesn't mean if you live in a rural community that we're actually at higher risk for cancer. It may mean that it's less access to prevention services, or screening, or treatment. And so we really want to address those issues.
Dr. Roy Jensen: What kind of services does MCA offer? I'm sure we just had a program all set to go and we just rolled it out and didn't consult anybody in this regard.
Dr. Krebill: Yes. That's exactly what we did. Not really. Our members are great. They're partners with us, and so they really tell us what is important to them as healthcare professionals, what their communities need. And from that, we try to develop something important to them. And so for example, many of you that are listening today may have participated in some of those programs. Smoking cessation has come up a lot, and so we now offer a televideo session for smoking cessation, a six week program. People come to their individual MCA member home and participate, and so that we may have like six or seven different communities at the same time participating in that. Others may have participated in our Pink Platoon, which is a cancer survivorship program, and that's a one day workshop. We go out and learn what's going on with individuals and their health as they're trying to thrive through cancer survivorship, and we have medical professionals and community members just having that discussion.Clinical trials, of course, is Gary's dream. That it would actually be something that we could get going, and our members are opening University of Kansas Cancer Center clinical trials right in their own home community, so people don't have to always travel in order to have access to those services. Finally, a lot of you think about second opinions, and if I have a cancer diagnosis, I would think about a second opinion at times as well, and so our members offer a way for people to come in and meet with University of Kansas Cancer Center physicians, and visit them via televideo, so they have a visit with the University of Kansas Physicians to really be assured that the care that they're getting is the right care for them at that time.
Dr. Roy Jensen: I can remember you and I, Dr. Doolittle, going out for probably about a year and a half-
Dr. Krebill: Right.
Dr. Roy Jensen: ... and listening to all of our centers and really getting them to tell us what they needed, as opposed to us tell them what they needed.
Dr. Doolittle: Right. I mean, I think there's really good medicine in the state of Kansas, and there's great cancer care in the state of Kansas. We really went out to set up a collaborative network, and one of the things that we heard loud and clear through the listening tour that went on for a year and a half was, "We want a greater association with the Medical Center. We would enjoy a higher level of collaboration than we've had." The clinical trials piece was big. As a medical oncologist, surgical radiation oncologist, clinical trials are part of our standard of care, and we have good docs in this state, and they want to be able to provide a standard for their patients as they would in an urban area.
And then I do think there was a vision at the Medical Center at the time that 85% to 90% of cancer patients in this country don't go to an NCI designated center. Practically that just can't happen, so we have to take what happens at a designated center and make sure that we diffuse information and gather information as we tailor programs for them.
Hope is entirely right. Every program that we've launched since the very beginning has come to us through a member site that had a need or had an idea. Nursing, social work, cancer registrars. That has actually been an interesting need that surfaced where they really need continuing ed, and one way they can get it is through the network.
Dr. Roy Jensen: We launched this effort in an attempt to really help cancer patients across this state. Could you give us some, either one of you, some specific examples of how the MCA has actually helped cancer patients?
Dr. Doolittle: We can talk in the clinical trials arena. Whether they're interventional trials for patients with a specific cancer, we offer a platform or protocols that are geared to the most common malignancies. And again, those are open based on what our member sites ask for. If you look at that in the last few years, over 1,000 patients have gone on either a cancer clinical trial that's interventional or population health study. What about the continuing ed work, Hope? I mean, that's huge.
Dr. Krebill: Yeah. Each year we provide about 3,000 continuing education credits to nurses, doctors, social workers, and cancer registers now. And I think that that really talks to or speaks to our healthcare providers in our state that care about evidence based medicine and want to have access to it, but traveling can be a real challenge for them. So if a physician leaves their community for a training in Hays, Kansas, they may have to leave for two or three days, versus just going for that one day of training. And so by offering the education right there at home via televideo and other ways, they're able to stay at home, see their patients, and get the continuing education that they want.
Dr. Roy Jensen: If you're just joining us, we're here with Dr. Gary Doolittle and Hope Krebill, and we're talking about the Midwest Cancer Alliance, which is the outreach network of the KU Cancer Center. Please remember to share this link with people you think might benefit from our discussion. Use the hashtag #BenchtoBedside.
What types of organizations or institutions are eligible to become an MCA member?
Dr. Krebill: Gary always says, "We have a big tent. Everyone's welcome." And what we say is, if you want to partner with us, if you want to make a difference in the health of your community, we're interested. And so the type of organizations that have joined us are, for example, Goodland, Kansas. And Goodland, many of you may recognize, it's the Van Gogh on I-70, about 17 miles from the border, and it's a community of about 5,000 people. But then we also have hospitals that are in larger communities across the state who have cancer centers with two or three colleges there every day. And then believe it or not, research organizations, and so as you know, K State and Stowers are also partners of the Midwest Cancer Alliance.
Dr. Roy Jensen: What specific benefits are there for member organizations in the MCA?
Dr. Doolittle: Please.
Dr. Krebill: I think it's really the community of practice. Imagine that you're a social worker in a community where you're the only social worker focused on oncology, or a research nurse where you're the only research nurse in your town. How do you learn to get better? It's by communicating with your colleagues. And so we've created networks so that members can connect with each other and really learn from each other. But of course you also do the hard numbers of just the number of screenings, and really being able to partner with their community to screen for cancer, and so that's another benefit.
Dr. Doolittle: I would echo some of Hope's comments. I spent a year in between training as an internist before I came back as a Hem/Onc Fellow. And I was in Leavenworth, Kansas for a year, and I'm very impressed with what it's like to be on the front lines, and having anything and everything walk in the door at any given time. And I was so used to an academic center where I could go down the hall and knock on a door and run a case by somebody, and I really noticed my role in the community and how different that was. And then as we come back and flash forward another 20 years, this whole idea of this collaborative practice or the community of practice, joining healthcare providers around the state and trying to address some of that isolation factor that you might experience out there. And we have some sites, whenever they call for a second opinion or they're presenting a patient at Tumor Board, I'm always nervous because I know it's going to be tough, because they manage cancer patients well and they bring us some of their more difficult cases. It's great for our trainees, but it's also good for them. They're not isolated. They have an opportunity to collaborate on that level.
Dr. Roy Jensen: I think one of the great reasons for the success of the MCS is frankly the two of you, and Gary, I suspect that there's not a single cancer doc across the state of Kansas that you don't personally know or have had some interaction with, either through they trained here with you, or you've shared a patient or whatnot, and I think that's been an incredibly valuable asset. And Hope, you've done a wonderful job in terms of, I think, understanding what the MCA is all about, what it can be, and making sure that the focus always stays on our member organizations and the patients that we jointly serve with them. So to me, that's the biggest reason why the MCA has had so much success, so thanks. Thanks for that.
Now, one thing that I suspect many of our viewers don't understand is, what role does the MCA play in our attaining and continuing on and becoming an NCI-designated comprehensive cancer center? Could both of you discuss that a little bit?
Dr. Doolittle: Yeah.
Dr. Krebill: Yeah.
Dr. Doolittle: Hope does such a good job with this piece of it. It's the whole community outreach and engagement portion of that, and I think we've known in Kansas for quite some time that there should be a focus on the rural sector, but now we're hearing from the NCI too that they feel like there should be a focus in the rural sector, and even part of the grant, when we look at becoming designated as a comprehensive center, there's this whole community outreach and engagement piece, and that makes the efforts of the Midwest Cancer Alliance and our partners even more important than before, I think. We feel like Hope's done a great job organizing this piece of it because it is a challenge. We're in a big center and there are a lot of moving parts, and we want to make sure that we let our partners know how things are moving forward and that they're a part of this process as well.
Dr. Krebill: Yeah. We serve all of the state of Kansas, as well as 18 counties in Missouri, and so NCI has asked us to really learn about what cancers are out there, what are the disparities, and then challenged us to really make a difference in those areas. And we can't do that as one organization. There's just no way, and so I think that's why MCA is really important to help us impact those cancers. We do it with our partners, we do it together, and there's just no way to serve that many people across all those miles without it.
Dr. Roy Jensen: One role that I know that you played, and you might tell our viewers a little bit about this, is you serve on what we call the Catchment Committee.
Dr. Krebill: Yes.
Dr. Doolittle: Could you discuss kind of how that relates to our center and NCI designation and serving the community?
Dr. Krebill: Sure. For the Catchment Committee, which that's a fancy word for the region we serve, and what we want to do is really understand the cancer. So just before I came here today, I was actually looking at the different cancer diagnosises. What are the highest number of cancer diagnosis in specific communities, as well as where their disparities? Are there some groups that have higher rates than others? And then the Catchment Committee helps to identify where we should be spending our time, what sort of research we should be doing as well. As in, what's important to our region? What should the researchers be thinking about so that we can really impact those cancers? So we don't decide what the research is or how to do it. We just say, "Hey, you know, there is a lot of breast cancer." Or, "There's a lot of colorectal cancer," and as a group we may decide that's an area that we want to focus on.
Dr. Doolittle: I think we've taken that another step too with our partners. Hope refers to the whole catchment area, and we're also looking at our MCA partners and their particular catchment area, and what their issues are individually as an organization, the people they serve. You can't improve upon things if you don't know what the baseline is. So a lot of it's about gathering proper data and then taking that and acting on it, developing a plan and acting and moving forward with it.
Dr. Krebill: And that is one of the expectations, right? That once we've identified and once KU has really done some interesting research on how to impact those cancers, then our job is to get that out into the community so that we can make a difference, not just here but across the state. And so that's the other part of the committee is looking at, "What are things that work? What sort of sun safety programs or tobacco cessation programs?" And we go out there and make sure that those programs that have been shown to work are happening across our state.
Dr. Roy Jensen: We've had a big focus on kind of our rural nature of our catchment area, but I would just mention that two of our really stalwart partners in the MCA have been Children's Mercy and Truman Medical Center. And maybe you could tell us a little bit about those two institutions.
Dr. Doolittle: They're really, as you can imagine, just with the populations they serve, they're very different organizations and the populations they serve are different. Children's brings a tremendous amount to the table. They were poised to move forward and really develop their research program. They had strong research, and now they're trying to elevate it further. They've been great partners. We've had multiple collaborative research projects that have been funded through the Midwest Cancer Alliance and the Partners Advisory Board, and that's enabled again, a greater level of collaboration between our two organizations, and then if you take a shift to Truman Medical Center, the population they serve is one that we feel is really important both for our community, but I also think on a national level, there's a strong push to make sure we're serving those in urban areas that are underserved, and that's where Truman does an excellent job with that, and they've been very open about protocol development and placing patients on study. You might want to talk about the Biobank, which I think is really unique and adds a tremendous amount both to our program but also on a national level.
Dr. Krebill: Yeah. Truman Medical Centers is an academic medical center and they have real interest in partnering on research, and so we have a biospecimen repository in partnership with them to be able to to collect data and specimen.
Dr. Doolittle: If we develop biobanks and we have tissue and we have blood samples, and new studies are developed and we need to test different disease types, the biobank enables us to go to it and access different cancers, different malignancies, different disease types.
Dr. Krebill: Truman Medical Centers has been a really strong partner in some of our population and cancer screening research. Colorectal cancer is really important to Truman. They have noticed that in their populations that they're serving, that there's a higher rate among African American me,n and so they want to do both service projects and partnership with us, but also participate in research. And I think that's a great example of where a partner has said to us, "We have an issue. We want to partner with you on research and we want to partner with you on service." And it works.
Dr. Roy Jensen: You know, I would give an example of the huge impact that that the MCA has had, is Children's Mercy. Children's Mercy was one of the founding members of the MCA, and I think through the funded research projects that were enabled through this partnership, through some experiences that they had in interacting with our Cancer Center, I honestly believe, and I think they'll tell you this, that that was a significant influence on their decision as an institution, to develop a children's research institute and recruit Tom Curran, who one of the world's most renowned biomedical researchers to come here and really change the entire direction of that institution. And I think in no small part that was due to their experience in the MCA, and the recognition on their part that they could take that whole institution to the next level.
Dr. Krebill: I think that's your vision, right? I mean, when you decided that the Midwest Cancer Alliance is an important piece of what should be part of our NCI designated cancer center, your idea about Children's Mercy and creating this Partners Advisory Board was amazing, because it really did move it to the next level, and now when we have meetings, lab meetings, MCA meetings, research meetings, you see KU researchers, Children's Mercy researchers all interacting, and you would not know there was a state line or separate organizations. We really are coming together as one team to really address cancer and really try to change how people experience it.
Dr. Roy Jensen: I'll see if Dr. Doolittle agrees with me on this, but I think one of the most important things that we recognized early on is the only way to be fair and equitable to every single member in the MCA is to treat them differently based on that particular institution's needs, and not try to have everybody conform to some formulaic approach to our interaction. To recognize and celebrate those differences, and view that diversity as a strength of the overall organization.
Dr. Doolittle: Yeah. No, I couldn't agree more, and Hope stated earlier, but we have organizations that are primary care hospitals that are in the far reaches of the state. We partner with Stowers, and one size doesn't fit all with us. We have really strong secondary hospitals that provide cancer care and have access to clinical trials that they wouldn't otherwise, and every site has their particular needs. In fact, when we bring a new site onboard, part of the onboarding process is that needs assessment. "What works for you?" Some of our sites had a strong need for navigation type services, and so we would address that piece. Some were more interested in the screening programs and the primary prevention piece, and it was a real important part of their individual cancer programs. So I couldn't agree more. It's really about fitting the needs, making the MCA fit the needs of the member organization.
Dr. Krebill: But I would also add that it's not just about us sending out things, or even just partnering with the local communities. We, as a cancer center, get by interacting with these individuals, with these members. They're the ones that will say to us as we're developing a new research trial to address cancer, they may say to us, "We don't have access to giving chemotherapy seven days a week." So if you're developing a drug study where that's a requirement, where it has to be seven days consecutively, 85% of individuals with cancer would not have access to it, and our members are always giving us that check. They're always letting us know, and joining conversations with researchers so that we really develop science and treatments that matter across the US, in rural communities, large communities, wherever. And so our members help us.
Dr. Doolittle: I think that's a really good point too, because you want the clinical trials work that you do and the outcome to be generalizable and to fit all populations. And I think the medical community, the oncologic community has done a good job in trying to recognize that we have to make sure we're offering these studies to underrepresented populations. I can even remember as far back as when they were saying, "You don't have enough women on your trials. Are you offering these trials to women of child ... When they were still of childbearing ages?" That was so long ago, but even since that time, making sure that we represent the population as a whole, that includes rural, that includes urban underserved.
Dr. Krebill: Sometimes we learn about ways to do good work, like HPV vaccination. So when you look around Hays Medical Center, that community there, their HPV vaccination rates, which is a vaccine that prevents cancer, is higher there than it is here, in communities that surround us. And so we're looking at that community and saying, "What are they doing differently? What can we learn from them so that we can bring that information back and try to make a difference here?"
Dr. Roy Jensen: The other thing I think we can break on a little bit is that the MCA has been discussed and been on panel sessions at the ACI, in terms of all the things that we've accomplished across this region. I think it has served as a model for how cancer centers can interact with their community, and I think the NCI has also taken note of these efforts and similar efforts across the country, because the new set of guidelines that have come out are actually going to have us highlight and discuss efforts like the MCA and how we're interacting with our community, and how do we approach problems within our community around cancer? And in that respect, I think we're really ahead of the curve and were ahead of the curve, and in fact, I know that I didn't tell you guys this for a couple of years, but our EAB told us to not do this.
Dr. Doolittle: I remember hearing about that, after you recruited me to be the medical director. A year and a half later, I heard. Full disclosure, Dr. Jensen.
Dr. Roy Jensen: Yes. Well, you know, you've got to keep the troops engaged and excited. You don't tell them that, "Well, the guys upstairs think we're all going to fail.
Dr. Krebill: [crosstalk 00:27:31] the door was open.
Dr. Roy Jensen: You certainly didn't fail, and I think you actually set the standard and moved the needle there, so congratulations on that. The other thing that's significant is the MCA, of course, recently celebrated their 10th anniversary. And as we approach the end of today's Bench to Bedside session, maybe could each of you share with us some of the accomplishments that the MCA has had over this last decade, what you're most proud of?
Dr. Krebill: Yeah. I think I'm most proud of is that the MCA continues to evolve based on what the members and the communities have said that they want. And so the smoking cessation programs that we started offering via televideo, the navigation support, and actually a national collaboration with AONN, the Academy of Oncology Nurse Navigators, has resulted from our navigation and our members requests for navigation resources. So that's what I'm proud of, is the evolution that continues to meet the needs of communities.
Dr. Doolittle: Couple things. I'm really proud of the collaborative spirit. I'm real impressed with our member sites. They come to our meetings regularly. They're outspoken, they're engaged, they're really a part of the whole process. So I'm really proud of that level of collaboration, and quite honestly I'm proud that we're still here. It's been 10 years, and as we watch what happens on the national scene and programs like ours come and go, and the fact that we're still here, I'm really proud of that. And I think it's a testament to the leadership from our end. I think it's a testament to the leadership at all of our sites as they've recognized this is an important effort.
Dr. Krebill: I remember eight years ago when Dr. Doolittle said, "We're going to start having monthly meetings with physicians at 5:00 on Monday, after a busy clinic day for all of them." And I went, "Mm-hmm (affirmative). Okay."
Dr. Doolittle: They actually show up.
Dr. Krebill: We turn on the TV. "Will they be there?" The first few times they would bring their work in with them and they didn't really look up a lot, and we were having a hard time looking up as well, and they show up every month, and they're engaged and they're talking to each other as well as to us, and yeah.
Dr. Doolittle: Yeah. We're part of that. We proud to be part of that.
Dr. Krebill: We are proud to be part of that.
Dr. Roy Jensen: One thing that I also think we should mention is our chief operating officer, Jeff [inaudible 00:30:18].
Dr. Krebill: Absolutely.
Dr. Roy Jensen: And during that year and a half when we were out canvassing the state and understanding what the needs were, Jeff was going beyond the state of Kansas and really looking at networks that many cancer centers had started or tried to start, and some of them had failed, and really did his due diligence around what works, what doesn't. And I think that was critically important to getting us off on the right foot, so we owe Jeff a huge [crosstalk 00:30:52].
Dr. Doolittle: Completely agree.
Dr. Krebill: Completely agree. And then the MCA team. We have a group of individuals that have been with the Cancer Center and with the MCA since the beginning. Brooke Groneman, Traci
McCarty. Soon we had Jim Coulter, and now we have Susan Krigel who is a psychologist, and Michelle Springer who works with clinical trials, and I'm doing the Oscar thing where I'm going to forget to mention my own mother.
Dr. Doolittle: Just as long as you get Kyla, Ashley.
Dr. Roy Jensen: Who are your kids?
Dr. Krebill: But everyone that has worked so hard, and that's really made a difference.
Dr. Roy Jensen: Well, in case the folks out there couldn't tell, this has been a labor of love for all of us, and NCI designation is a nice recognition, but if you're not connecting with your cancer patients in the population that you serve, then it's all just kind of a wasted effort. So I think the MCA helps us make sure that you know, we're doing the right thing. So thank you.
Dr. Krebill: Thank you.
Dr. Doolittle: Thank you.
Dr. Roy Jensen: Thank you, Gary. That's it for today. For more information on the Midwest Cancer Alliance, please visit www.midwestcanceralliance.org. We appreciate you joining us, and we invite you to tune in next week, Wednesday at 10:00 AM, for Bench to Bedside. Thanks for watching.
About MCA
MCA is a network of hospitals and physician groups located throughout The University of Kansas Cancer Center’s catchment area. Working together, we leverage unique regional resources to promote and translate the latest evidence-based clinical and community health practices for patients close to their homes. Team members also collaborate with local members to enhance their research infrastructure and to proactively execute cancer prevention and control strategies to decrease the burden of cancer in the catchment area.
Clinical trials
MCA collaborates with The University of Kansas Cancer Center to offer MCA clinical research partners access to advanced clinical trials. This is an integral component to reducing cancer disparities. A study of nearly 37,000 participants found that urban and rural cancer patients had similar survival outcomes when they were enrolled in a clinical trial.
A new mobile application developed by KU Cancer Center makes it easier for physicians to find clinical trial opportunities for their patients. Learn more.

Cancer screenings
Each year, MCA hosts several cancer screening events throughout the region. Services at these events such as skin cancer checks, prostate cancer screenings and colon cancer screening kits are offered at no charge to the public. Since 2008, more than 10,000 individuals have attended an MCA screening. In 2018, of the 1,673 individuals who were screened, nearly 300 were referred to a physician due to abnormal findings.
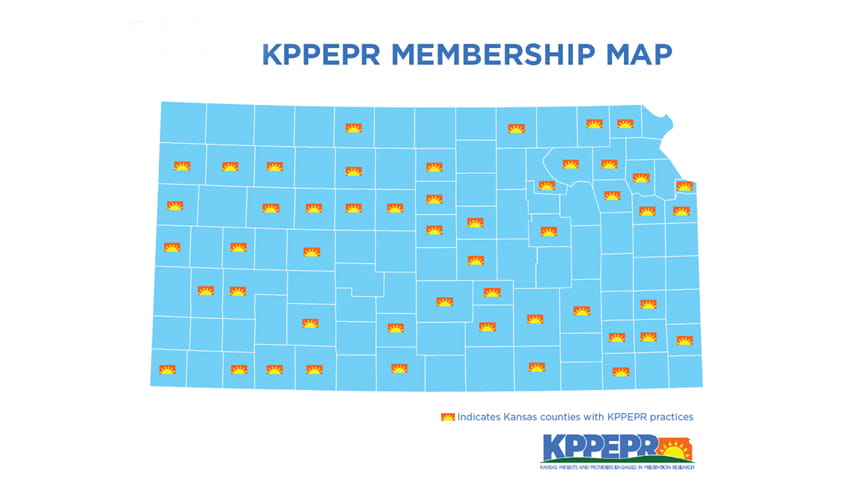
Kansas Patients and Providers Engaged in Prevention Research (KPPEPR)
The Kansas Patients and Providers Engaged in Prevention Research (KPPEPR) network is a practice-based research network of patients, clinicians, primary care practices, hospitals and public health organizations located in geographically diverse communities across rural Kansas. The mission of KPPEPR is to conduct collaborative, interdisciplinary community-based research to promote the health of Kansans and enhance primary care practice.
KPPEPR accelerates the movement of scientific discoveries into practical applications that benefit patients, communities and the healthcare system. KPPEPR research focuses on promoting health through prevention, behavior change, early diagnosis and treatment. This network of more than 75 primary care practices expands our ability to conduct trials and implementation research focused at the level of the primary care practitioner.
KPPEPR is one of the first-of-its-kind networks in the nation to build research partnerships between clinicians, patients, public health professionals and academic researchers.
Continuing education
Annually, MCA provides more than 2,000 continuing education credits on average to nurses, doctors, social workers and registrars. The MCA is committed to bringing the latest information on cancer research and care to its members. Various events are available in person or via teleconferencing so that healthcare professionals can stay close to home, near their families and patients.
Partners Advisory Board
The Masonic Cancer Alliance’s Partners Advisory Board purpose is to assist with the pursuit and maintenance of The University of Kansas Cancer Center's National Cancer Institute designation by demonstrating research and education collaboration among key hospitals and research institutions for the benefit of the region. The MCA Partners Advisory Board serves in an advisory capacity to the director of The University of Kansas Cancer Center and CEO of the Masonic Cancer Alliance, Roy Jensen, MD, and executive director of the Masonic Cancer Alliance, Hope Krebill.
For more than 10 years, MCA’s Partners Advisory Board members have championed collaborative research and provided substantial financial support for new research initiatives. New research projects initiated by Children’s Mercy Kansas City via the MCA Partners Advisory Board since 2010 are excellent examples of these efforts. These studies have ranged from studying tumors to understanding the needs of adult survivors of pediatric cancers. The MCA Partners Advisory Board is committed to advancing research and clinical trial access across the Heartland.