- Home
- Types & Treatments
- Brain Cancer
- Treatments
Brain Cancer
Brain Cancer Treatment
Once the diagnosis of brain cancer is made, you and your family can be faced with many difficult decisions to make about your brain cancer treatment options. Factors to consider include the extent of resection (how much of the tumor was removed during surgery), type of tumor and status of important markers like chromosomes or enzymes, your ability to function and your age.
The most important factor in determining a treatment course is to consider your wishes and willingness to accept different levels of side effects in order to benefit from the treatment. When your care team recommends a treatment, they will listen to you, respect your decisions and walk the journey with you.
Brain Cancer Treatment Options
Your care team’s job is to fully describe your brain tumor treatment options, including the risks and benefits of each. Before recommending treatments, we will need to review records of medical care that you have previously received from any care provider.
This includes MRI scans, treatment history and full pathology, which may lead to a request for our neuropathologist to give a second opinion of the tumor specimen. This review allows us to present the full range of appropriate treatment options for you. Our tumor board, which includes specialists from neurosurgery, neuroradiology, neuropathology, radiation oncology and neuro-oncology, will discuss MRI scans and pathology findings together to collaborate on a recommendation for treatment.
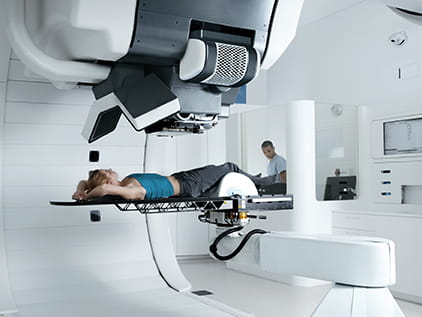
Proton therapy in Kansas City
Receive lifesaving proton therapy treatment from the region's most experienced team of proton experts.
Life after brain cancer
Surviving cancer is a lifelong process. Each person faces different challenges physically, cognitively and emotionally together with their families. Your care team will often recommend regular checkups and MRI scans. At these visits, we can continue to help address any of the ongoing symptoms of either tumor or treatment.

More options, more hope
Many new therapies are available through clinical trials. Find out how you may benefit from a clinical trial, and what it can do for others.
Start your path today.
Your journey to health starts here. Call 913-588-1227 or request an appointment at The University of Kansas Cancer Center.